Athletic Medicine is moving!!!
Hello Followers and Subscribers:
AthleticMedicine.WordPress.com will soon become Stoneathleticmedicine.com. I just have a few more administrative details to get through such as redirects and establishing links. The move will become official within a week, however, the site is up and running. You can visit and subscribe now!
Moving to my own domain is long overdue. I have nearly 900 email subscribers and almost 2,000 total followers. I am honored to have had such great success and look forward to continued blogging. Followers can expect the same content with a different look and feel.
What do you need to do? For most of you, nothing! I will take care of everything. Most will remain as subscribers, followers and will continue to receive alerts when new content is posted. WordPress.com bloggers who have signed up for email notification, you will need to sign up again.
Thanks again to all of you who have helped me grow!
All the best! Josh
“Coaches have used my “RICE” guideline for decades, but now it appears that both Ice and complete Rest may delay healing, instead of helping.” – Gabe Mirkin, MD, March 2014
In 1978, Gabe Mirkin, MD coined the term RICE. Health care practitioners to laypersons are quick to recognize RICE as the ‘gold standard’ treatment option following injury. Followers of my blog know my stance against ice and now there is support from the physician who coined the term. Yes, the very same physician, Dr. Gabe Mirkin, who coined RICE, is now taking a step back. I reached out to Dr. Mirkin and asked for permission to share his story. As you will read below in Dr. Mirkin’s full post, the lack of evidence for cryotherapy is something we must listen to.
 This is a controversial topic. My blog Why Ice and Anti-inflammatory Medication is NOT the Answer sparked a lot of debate. I had nearly 30,000 page hits per day for several weeks. I recently received a tweet from a peer (@AlanMRussell) who attended a presentation by Cindy Trowbridge from the University of Texas-Arlington refuting many of my comments. The debate continues, but given the evidence – or lack thereof – I stand by my thoughts that ice does not facilitate tissue healing.
This is a controversial topic. My blog Why Ice and Anti-inflammatory Medication is NOT the Answer sparked a lot of debate. I had nearly 30,000 page hits per day for several weeks. I recently received a tweet from a peer (@AlanMRussell) who attended a presentation by Cindy Trowbridge from the University of Texas-Arlington refuting many of my comments. The debate continues, but given the evidence – or lack thereof – I stand by my thoughts that ice does not facilitate tissue healing.
I recently had the pleasure of connecting with Nichan “Nick” Zourikian a physiotherapist and researcher at Sainte-Justine University Hospital Center in Quebec. Nick published a study with Angela Forsyth, DPT (Rush University Medical Center) that led to a unique, in-journal debate among experts. The original review article published in Haemophilia, challenged the effectiveness of ice (1). This led to a “Letter to the Editor” rebuttal published one year later (2), which led to a rebuttal to the rebuttal published in the same journal (3). Why is this such a hot topic? Nick summed it up perfectly in an email:
“There clearly exists a dogmatic polarization on the use of ice in our physiotherapist/athletic therapist communities! Old habits die hard. Many colleagues (even in our hemophilia community) still insist on using ice…despite the current scientific evidence available.” Nick is spot on, RICE is an old habit that is dying hard.
I have long said modalities are overused and exercise is under used. Ice: The Overused Modality was my first post to make this point. I have added several posts that demonstrate the need for exercise and the positive effect mechanical load has on tissue healing and repair. See my posts on Mechanotransduction, Achilles Tendinopathy and reversibility as these explain more.
The NATA’s position statement in August 2013 on management of ankle sprains would support my anti-ice case. The researchers for the NATA position statements take years to critically appraising data to make conclusions. They comb over all the data and rate evidence from best “A” to worst “C”. In this particular position statement cryotherapy was overall a C rating for evidence (4). The article says “Strong clinical evidence for advocating cryotherapy is limited”. The evidence that had the better ratings: functional rehabilitation, proprioception, balance, and range of motion (note: these are all tissue loading exercises) (4). What’s interesting is many of the readers to my blog are athletic trainers, physical therapists, and physiotherapists. Yet, they are the ones who think I am nuts. Your own organization has a comprehensive position statement that supports my thoughts. Am I that crazy?
I read a piece on Medscape the lead author of the NATA position statement, Thomas W. Kaminski, PhD, ATC, said that he believes that many practitioners are still following the prescription too closely (5). The article goes on to quote Dr. Kaminski: “I wish I could say that what we found is what is really being done in a clinical setting.” There is another quote: “Maybe our European colleagues know something we don’t”…”there is very little icing over there.” (5)
Despite the lack of evidence advocating the use of ice the debate continues. Peers continually challenge me and would like to see me hung, drawn, and quartered for suggesting no ice. ‘My gosh, you mean I shouldn’t take 30 ice bags out to the baseball field wrap shoulder and elbows? You’re insane!’ A shift in paradigmatic treatment is on the horizon. Exercise is heating up and ice is melting down. Below is the full article from Dr. Mirkin’s website, which will only fuel the end of the ice age.
****************************************************
March 20, 2014
by Gabe Mirkin, MD
When I wrote my best-selling Sportsmedicine Book in 1978, I coined the term RICE (Rest, Ice, Compression,Elevation) for the treatment of athletic injuries (Little Brown and Co., page 94). Ice has been a standard treatment for injuries and sore muscles because it helps to relieve pain caused by injured tissue. Coaches have used my “RICE” guideline for decades, but now it appears that both Ice and complete Rest may delay healing, instead of helping.
In a recent study, athletes were told to exercise so intensely that they developed severe muscle damage that caused extensive muscle soreness. Although cooling delayed swelling, it did not hasten recovery from this muscle damage (The American Journal of Sports Medicine, June 2013). A summary of 22 scientific articles found almost no evidence that ice and compression hastened healing over the use of compression alone, although ice plus exercise may marginally help to heal ankle sprains (The American Journal of Sports Medicine, January, 2004;32(1):251-261).
Healing Requires Inflammation
When you damage tissue through trauma or develop muscle soreness by exercising very intensely, you heal by using your immunity, the same biological mechanisms that you use to kill germs. This is called inflammation. When germs get into your body, your immunity sends cells and proteins into the infected area to kill the germs. When muscles and other tissues are damaged, your immunity sends the same inflammatory cells to the damaged tissue to promote healing. The response to both infection and tissue damage is the same. Inflammatory cells rush to injured tissue to start the healing process (Journal of American Academy of Orthopedic Surgeons, Vol 7, No 5, 1999). The inflammatory cells called macrophages release a hormone called Insulin-like growth Factor (IGF-1) into the damaged tissues, which helps muscles and other injured parts to heal. However, applying ice to reduce swelling actually delays healing by preventing the body from releasing IGF-1.
The authors of one study used two groups of mice, with one group genetically altered so they could not form the normally expected inflammatory response to injury. The other group was able to respond normally. The scientists then injected barium chloride into muscles to damage them. The muscles of the mice that could not form the expected immune response to injury did not heal, while mice with normal immunities healed quickly. The mice that healed had very large amounts of IGF-1 in their damaged muscles, while the mice that could not heal had almost no IGF-1. (Federation of American Societies for Experimental Biology, November 2010).
Ice Keeps Healing Cells from Entering Injured Tissue
Applying ice to injured tissue causes blood vessels near the injury to constrict and shut off the blood flow that brings in the healing cells of inflammation (Knee Surg Sports Traumatol Arthrosc, published online Feb 23, 2014). The blood vessels do not open again for many hours after the ice was applied. This decreased blood flow can cause the tissue to die from decreased blood flow and can even cause permanent nerve damage.
Anything That Reduces Inflammation Also Delays Healing
Anything that reduces your immune response will also delay muscle healing. Thus, healing is delayed by:
Ice Also Reduces Strength, Speed, Endurance and Coordination
Ice is often used as short-term treatment to help injured athletes get back into a game. The cooling may help to decrease pain, but it interferes with the athlete’s strength, speed, endurance and coordination (Sports Med, Nov 28, 2011). In this review, a search of the medical literature found 35 studies on the effects of cooling . Most of the studies used cooling for more than 20 minutes, and most reported that immediately after cooling, there was a decrease in strength, speed, power and agility-based running. A short re-warming period returned the strength, speed and coordination. The authors recommend that if cooling is done at all to limit swelling, it should be done for less than five minutes, followed by progressive warming prior to returning to play.
My Recommendations
If you are injured, stop exercising immediately. If the pain is severe, if you are unable to move or if you are confused or lose even momentary consciousness, you should be checked to see if you require emergency medical attention. Open wounds should be cleaned and checked. If possible, elevate the injured part to use gravity to help minimize swelling. A person experienced in treating sports injuries should determine that no bones are broken and that movement will not increase damage. If the injury is limited to muscles or other soft tissue, a doctor, trainer or coach may apply a compression bandage. Since applying ice to an injury has been shown to reduce pain, it is acceptable to cool an injured part for short periods soon after the injury occurs. You could apply the ice for up to 10 minutes, remove it for 20 minutes, and repeat the 10 minute application once or twice. There is no reason to apply ice more than six hours after you have injured yourself.
If the injury is severe, follow your doctor’s advice on rehabilitation. With minor injuries, you can usually begin rehabilitation the next day. You can move and use the injured part as long as the movement does not increase the pain and discomfort. Get back to your sport as soon as you can do so without pain.
*****************************
I want to thank Dr. Mirkin for allowing me to share his article. I really appreciate his continued contributions to health and wellness.
Until next time –
Josh
References:

I AM A CERTIFIED ATHLETIC TRAINER! RESPECT ME! LOVE ME! HONOR ME!
It’s not often I completely take a post from another, but Mr. Yusuf Boyd, of Biomechaniks in Tennessee and North Carolina wrote a post last week that was on point! While I do not agree with everything in the post, what he says has a lot of merit and is worthy of a share.
I love Athletic Training and my fellow Athletic Trainers, but honestly this is the whiniest group on the face of the planet. March is National Athletic Training month; slogans fill my twitter feed: “I love my Athletic Trainer”, “Athletic Trainers’ save lives”, “My Athletic Trainer has my back.” Great, I am glad we are a prideful bunch, but enough of this holier-than-thou attitude. All I hear is “I am a Certified Athletic Trainer! I deserve respect!” It sounds like a crying toddler who didn’t get a lollipop from the dentist.
This very profession that demands respect also has many of its constituents complaining about the BOC’s new Evidence Based Practice CEU requirements. Really, you want more respect, but will moan and complain when our certifying agency and association wants higher standards?
This post is going to aggravate many. Those agitated are not hearing what I am saying. You do deserve respect. I am for promoting the profession. I appreciate the efforts of the PAC, but you don’t get it by crying from the rooftops. You earn it. If you do a good job you will get your respect. What follows is Yusuf’s post. Enjoy.
*******************************************
A LETTER TO ATHLETIC TRAINERS
Written by Admin
Every year around March I post something related to our wonderful profession, 2014 will be no different. The time has come to stop whining about how you are addressed and be more concerned about how well you do your job. Do you know what your job is? Are you fully aware of your skill set? If I asked one hundred AT’s this question, I am sure all would say yes but I’ll bet the majority of them still treat injuries like it is 1991…taping ankles and stretching hamstrings. I am far from being the best but I have learned a few things over my 15 + years in the profession and it frightens me when I look at my twitter feed, the concern is not about being a better AT but being recognized as more than just a trainer. This has been a topic of discussion for years and I am sure it will continue to be for more to come but how about taking a different approach. How about actually going out there and helping individuals get better through proper technique learned from reading research and discussions with individuals who know how to fix problems instead of placing bandaids on injuries? Taping ankles does not prevent ankle sprains, you can teach a monkey to tape an ankle, fill a water cooler, and drive a gator.
Our skill set is very unique within the realm of allied health care but yet we do not take full advantage of it. We complain about lack of respect, job availability, and pay but we do nothing to separate ourselves and show our true worth. It amazes me that in a profession where applied techniques should rule, they do not and we lean more on the latest modalities, etc. I need a Hivamat, cold laser, Normatec, the old faithful e-stim and ultrasound. These devices have their place with acute issues but the majority of cases we manage are a result of overuse. I was fortunate enough to attend a great ATEP program which promoted independent thought, I was even more fortunate to work in pro sports for several years and learn from some of the best in the business. Both experiences helped shape the AT I am today but they also take the back seat to me understanding what my job description is and what I need to do to ensure that I make every effort to excel at it everyday. For those who may need it, here is a reminder as listed on the NATA’s website and in this document:
Athletic trainers (ATs) are healthcare professionals who collaborate with physicians. The services provided by ATs comprise prevention, emergency care, clinical diagnosis, therapeutic intervention and rehabilitation of injuries and medical conditions.
Athletic trainers deliver rehabilitation services under a physician’s guidelines.
Guidelines are general directions and descriptions that lead to the final outcome, thereby allowing the athletic trainer to rely on clinical decision making in constructing the rehabilitation protocol. Protocol are rigid step-by-step instructions that are common in technical fields and do not allow flexibility and/or clinical decision making.
Athletic trainers function under a physician’s direction.
The terms “direction” and “supervision” mean two different things. Most importantly, supervision may require the on-site physical presence of the physician and that the physician examines each and every patient treated by an athletic trainer. Direction, on the other hand, requires contact and interaction, but not necessarily physical presence.
Lets break this down:
“Athletic trainers (ATs) are healthcare professionals who collaborate with physicians.”
If you operate independently this is more important than anything, you must establish a relationship with a physician, preferably an orthopedic. It validates your existence and if you are good at what you do you will get referrals. Without a physician it will be difficult to use many of your skills legally. Thank goodness for state licensure.
The services provided by ATs comprise prevention, emergency care, clinical diagnosis, therapeutic intervention and rehabilitation of injuries and medical conditions.
What is prevention? In my opinion for the AT, it should be defined as: reducing the risk of sport-related injury through early diagnosis and treatment; and recognition of limitations and rehabilitation potential. This definition encompasses everything but emergency care and certain medical conditions and if followed properly, truly reduces chance of injury. The key phrase in NATA’s definition of an AT though is “therapeutic intervention and rehabilitation of injuries”. Therapeutic intervention in my eyes is hands on care to achieve a desired outcome. Does taping an ankle fall within those guidelines? In my humble opinion, no, but measuring ankle dorsiflexion, assessing rear foot angle, and testing hip strength does (there’s a lot of research on correlation between hip strength and ankle instability). Another example would be the unwritten rule of stretching hamstrings because a patient/client says they feel “tight” without proper assessment. More often than not, the hamstrings are synergistically dominant due to an anterior pelvic tilt and reciprocal inhibition of the glutes. This may cause one to say their hamstrings “feel tight” which they are, but they are elongated under tension as a result of misalignment of the pelvis, not short and contracted. In this case, it is more appropriate to stretch the hip flexors and activate the glutes. It is this type of evaluation that prevents injury; early diagnosis and recognition of the musculoskeletal warning signs, in other words, therapeutic intervention.
Recreational, amateur, and professional athletes
As an athletic trainer you may be in either of the settings listed above, respect only comes to those that earn it. If you work with athletes and they are always in front of you with the same issue, there is something you are doing incorrectly. My patients range in age from 11 – 81 years and compete at levels from recreational to professional. The approach taken to treating those musculoskeletal injuries does not differ because of age, setting, or level of competition. For those individuals in a strength & conditioning/fitness/performance enhancement role, if you are not the busiest individual in your place of practice something is wrong. You have the skills to not only address fitness, but to also deal with any musculoskeletal issues…use that to your advantage. Assess your clients as if you are in the athletic training room and then put them on a plan to move better, their performance will increase. You may say, but I do this….do you really, or do you just tell people you do? If you properly diagnose and follow appropriate protocol, not diverting because you are bored with it or you think they have progressed when they have not, then great! But most do not fall within this category. A colleague recently posted a blog on sticking with your plan, it is worth a read. Click here.
I choose a soft science for my graduate education because I felt it would make me better at rehabilitation and I must say it does. We get so wrapped up in returning an individual to playing status that we overlook one of our main responsibilities which is to protect the athlete. If you do not fix the problem and only bandaid it, you are not protecting the athlete, you are just adding to the problem. There is substantial research out there to back this, I wrote a short blog on it a while back, it can be found here.
The ability to work under the direction of a physician is a great responsibility, one that must not be taken lightly. There are too many individuals who worked too hard to get this profession to its current level for it to be compromised by individuals who are just lazy and want everything handed to them. As I stated in the beginning, I do not claim to know it all and I never will simply because I learn something new everyday. Every patient is an opportunity for me to learn something different about how the musculoskeletal system works from a functional perspective. If you do not have a comprehensive understanding of functional anatomy, get on that ASAP! There was a huge factor left out of your A & P class that most overlook. The cadaver was prone or supine on a table, the class did not address how everything changes once the kinetic chain closes. You have to open your mind to a different way of thinking, you have the knowledge, just apply it!
Yusuf Boyd, M.S., ATC, LAT, CES, PES, CKTP
************************************************
Thanks Yusuf for writing this. It takes guts to go against the majority. I invite you all to visit Yusuf’s company page. You can also find him on twitter @BIOMechaniks.
How many times have you racked your head wondering; why is this not getting better? How come they’re still in pain? How do we have all of this evidence and knowledge at our disposal, yet individuals do not respond as anticipated? The science says, for injury ‘Z’ treat with ‘X’ and rehabilitate with ‘Y’, yet when we apply those tools they don’t work? Why are they not getting better? What are you doing wrong? What are they doing wrong?
Often times we immediately point the finger in the wrong direction. First we think, “There must be something else wrong that I missed during my evaluation.” Another is “Well, [the patient] must be doing something that I told him/her to avoid.” Also, “Let’s try doing this instead.” For readers of this blog who are health care practitioners, how many times have you said one of the above lines when therapy failed?
While it is not wrong to ask the above questions, these shouldn’t be the first questions you ask. First you need to make sure you and the client are upholding the three C’s: 1.) Consistency. 2.) Commitment. 3.) Correctness. Let me explain how all of these are needed to have optimal outcomes.
Consistency:
Once you have identified the problem and developed a treatment plan, you must consistently and religiously follow the plan. Lack of consistency is one of the problems with standard outpatient care. How can patients get better with 2-3 visits per week? How can they improve when insurance lapses after 12 visits? There are 168 hours in a week; spending < 2% of that time in therapy will not elicit the desired outcomes. As practitioners we must continually attack the underlying problem. Many of the chronic conditions we face are a result of learned patterns. The only way to break the cycle is to continually teach the body what it needs to do.
Commitment:
Both clinician and client must be committed to the plan. How many times have you provided clients clear directions of what to do / not do, only to hear “Yes, I did as you told, but I did go to Zumba” … “Yes, but I did go hiking” … “Yes, but I read online I should do [stretches], so I tried them.” You’re left just shaking your head.
Practitioners: don’t let your head grow bigger, you’re worse than the patients. Practitioners continually seek the best for their clients. The problem is that practitioners are impatient. The first sign of adversity, or delay in expectations, you begin seeking alternative treatment. Remember it takes 4-6 weeks minimum to obtain desired adaptations. Stay the course, don’t quit the plan!
Correctness:
Correctness, or perfection, comes in to play during execution of exercise. If you’re not performing the exercise to perfection, then you might as well not be doing it all. A friend recently asked me, ”Why the term of corrective exercise? Shouldn’t all exercise be corrective?” I said, “No, exercise is movement. Corrective exercise is perfect movement.”
Our bodies are masters of cheating. I can ask 10 people to squat and each person will have a slight variation to the squat. Limited dorsiflexion, glute weakness, tonicity through the posterior oblique fascial line, overactive iliopsoas, and I could go on; all will have a subtle impact on movement because of the body’s way of cheating and taking the path of least resistance.
Similarly, when a client is asked to perform a rehabilitation exercise, the body can and will compensate. The practitioner must watch for and immediately correct any sign of compensatory movement. Performing the exercise improperly can create more problems than not doing the exercise at all.
Summary:
You can have all the gadgets and gizmos in your arsenal to treat. You can have the alphabet soup of credentials after your name. But in my humbled opinion, none of it matters if you do not practice consistency, stay committed to the plan, all while having absolute correctness. Doing so will give you the best opportunity for rehabilitation success.
When we think of running injuries we immediately think lower extremity, IT Band syndrome, Patellofemoral Pain Syndrome, Achilles Tendinopathy, Medial Tibial Stress Syndrome, Plantar Fasciitis, and the like. However, one of the most common and debilitating injuries in runners is low back pain. So why are runners so at risk of developing low back pain? Most musculoskeletal injuries are multifactorial, but more often than not many chronic injuries result from underlying movement dysfunction.
Vladamir Janda (1928-2002) revolutionized human movement dysfunction and rehabilitation in 1979 when he described three compensatory movement syndromes. These syndromes were a result of pattern overload (i.e. running) and static posturing. Janda recognized that certain muscles were prone to weakness while others were overactive. He continually investigated these movement syndromes and later learned that the muscle imbalances were systematic, predictable, involved the entire body, and a common cause of injury.
Since Janda introduced this topic research has continued to answer what and why questions surrounding these compensatory patterns. We have learned hypertonic / hypotonic muscles and the delicate interplay they have on integrated functional movement. For those who have developed low back pain, I’d like to highlight three specific muscle battles that can be found in many individuals with low back pain. It is a battle of muscle supremacy, good vs evil, where evil prevails and injury trails.
Battle 1: Glute Medius (Good) vs Tensor Fascia Latae (Evil)

 While both the glute medius and Tensor Fascia
While both the glute medius and Tensor Fascia
Latae (TFL) work synergistically to generate hip abduction, the glute medius provides femoral external rotation while the TFL does internal rotation. Additionally, the TFL is a hip flexor while the glute medius is a hip extensor. The problem is the TFL often wins the battle of supremacy of these two. The hypertonicity of the TFL and hypotonicity of the glute medius results in excessive femoral internal rotation, excessive hip flexion, and excessive anterior tilting of the pelvis.
Battle 2: Glute Max (Good) vs. Iliopsoas (Psoas Major and Iliacus) (Evil)
 Early in Janda’s study he found subjects without activity in the gluteus maximus during hip
Early in Janda’s study he found subjects without activity in the gluteus maximus during hip  extension movements. This is what actually formed a lot of his later work. The glute max and iliopsoas are true antagonists of one another. The glute is responsible for hip extension, external rotation, posterior pelvic tilt, and to a small degree, hip abduction. The iliopsoas is a strong hip flexor, with external rotation, trunk flexion, lateral trunk flexion, hip adduction and anterior pelvic tilt. The Iliopsoas wins the battle of supremacy. The outcome of this battle is anterior pelvic tilt, increased lordosis, hip flexion and hip adduction.
extension movements. This is what actually formed a lot of his later work. The glute max and iliopsoas are true antagonists of one another. The glute is responsible for hip extension, external rotation, posterior pelvic tilt, and to a small degree, hip abduction. The iliopsoas is a strong hip flexor, with external rotation, trunk flexion, lateral trunk flexion, hip adduction and anterior pelvic tilt. The Iliopsoas wins the battle of supremacy. The outcome of this battle is anterior pelvic tilt, increased lordosis, hip flexion and hip adduction.
Battle3: Intrinsic Core Stabilizers (Good) vs. Erector Spinae (Evil)
 The erector spinae, as the name indicates, extends the spine. The erector spinae is also
The erector spinae, as the name indicates, extends the spine. The erector spinae is also 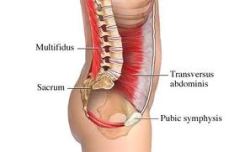 responsible for anterior pelvic tilting, and will laterally flex and posteriorly rotate the spine to the left or right when activated unilaterally. The intrinsic core stabilizers have a lot of muscles—transverse abdominus, internal oblique, transversospinalis group (multifidi, rotatores, semispinalis, interspinalis and intertransversarii), and pelvic floor muscles—far too many to type out the isolated functions of each, but as a unit, they stabilize the spine and pelvis. Evil wins again, resulting in spinal instability, increased spine lordosis, and anterior tilting of the pelvis.
responsible for anterior pelvic tilting, and will laterally flex and posteriorly rotate the spine to the left or right when activated unilaterally. The intrinsic core stabilizers have a lot of muscles—transverse abdominus, internal oblique, transversospinalis group (multifidi, rotatores, semispinalis, interspinalis and intertransversarii), and pelvic floor muscles—far too many to type out the isolated functions of each, but as a unit, they stabilize the spine and pelvis. Evil wins again, resulting in spinal instability, increased spine lordosis, and anterior tilting of the pelvis.
Outcomes:
When combining the repetitive motion of running with static posturing associated with daily living, evil is able to dominate good. Secondary to our repetitive motion of runners, coupled with static posturing of our activities of daily living, evil has been allowed to dominate good. So, what is the final outcome if evil continues to prevail? We develop movement impairment syndromes that bring about a significant risk of injury, including low back pain.
It’s time to take charge and inhibit the evil-doers from dominating human movement. Through corrective training we can bring calmness over the evil and raise morale of the good. Hopefully, we can bring these two groups together and work harmoniously. In doing so, runners can work toward optimal movement efficiency thereby preventing injury and improving performance.
**If you have musculoskeletal pain that you think may be a result of movement impairment syndrome, please contact me for a free evaluation.
Overview and etiology:
The term “tendinitis” or any [insert any body part] with “itis” is tossed around as if it is the only possible cause for musculoskeletal pain. However, the “itis” is not really true. A tendon, specifically the Achilles tendon, is not really inflamed, rather it is deranged (tendiopathic / tendinopathy). In January 2013 the Annals of Human Genetics published an article that demonstrated Achilles Tendinopathy is associated with gene polymorphism (Abrahams, et al., 2013). COL51A is a gene that encodes the development and organization of Type V collagen. This collagen can be found in ligaments, tendons, and connective tissue. COL51A plays an integral role in development and maintenance of connective tissue. Abrahams, et al. (2013) demonstrated that polymorphisms occur in the COL51A gene causing altered structure of collagen resulting in tendinopathy.
The tendon may become fusiform or thickened, but it is due to cellular derangement rather than inflammation. Kannus and Jozsa in a controlled study of 891 patients with Achilles tendon rupture found that 97% of patients had degenerative changes in the ruptured tendon. The study also found that 34% of asymptomatic tendons also had degenerative changes (2)
In tendinopathic tissue the collagen formation becomes deranged through sedentary lifestyle, excessive activity, and poor neuromuscular alignment and coupling. Couppe´, Kongsgaard, et. al, looked at effects of habitual loading in elite badminton and fencers athletes and found that the tendon will undergo hypertrophy and increased stiffness with excessive loading (3). Another study found that immobilization led to decreased mechanical properties of the tendon, while exercise increased mechanical properties (4). If there is movement impairment centralized within the foot and ankle region, such as rearfoot eversion or tibial external rotation it can lead to various symptomatic responses, including plantar fasciitis, medial tibial stress syndrome and Achilles tendinopathy (5).
Appropriate loading and exercise:
Excessive loading and sedentary lifestyle may lead to tendinopathy of the Achilles tendon, so there is a sweet spot – not too much and not too little. A systematic review in 2012 found that removing athletes from competition is not beneficial for treatment of tendinopathy (6).
Eccentric exercise has been recommended in the treatment of tendinopathy for more than 30 years. Evidence supporting the use of eccentric exercise in treatment of tendinopathy is well-documented and strong. A systematic review published in 2012 found eccentric loading to be beneficial for treatment of Achilles tendinopathy (7). Murtaugh and Ihm demonstrated that eccentric exercises can be effective in the treatment of tendinopathies at various locations of the body (8). The authors also found that performing sets of 15 repetitions of each exercise 1-2 times daily has the greatest benefit.

Correction common movement dysfunctions, such as knee adduction, tibial external rotation, and foot external rotation can go a long way in preventing Achilles tendinopathy.
Clark and Lucett demonstrated that corrective lower extremity muscular imbalance training and enhancing neuromuscular coupling can reduce lower extremity injury (9). Inhibiting overactivity of the peroneals, lateral gastrocnemius and biceps femoris, while simultaneously reversing hypotonicity of the medial gastrocnemius, anterior / posterior tibialis, and medial hamstrings can correct foot and ankle malalignment. Correcting these dysfunctional movement patterns can improve Achilles tendinopathy.
Why does exercise work? Physiology of Loading:
Therapeutic exercise has traditionally been used to restore range of motion, increase strength and enhance functional movement. However, it is becoming more apparent that exercise stimulates tissue regeneration. Following the principles of mechanotransduction, the passage of forces generated through movement from cells to cell nuclei plays an important role in tissue repair. Clinical research is advancing understanding of how to best load tendon to facilitate repair. However, the differentiation of stem or progenitor cells and increases in fibroblast is needed to maintain homeostasis and for repair of tendons, cartilage, bone and ligaments. Appropriate load can stimulate progenitor cells and regeneration collagen tissue in the Achilles tendon as well as other tendons.
The issue of tendon and tendinopathy provides unique perspective to this discussion of therapeutic exercise and mechanobiology. The original rehabilitation protocols developed when tendinopathy was viewed as tendinitis – long before mechanobiology emerged – are no longer relevant. Obviously there is not a one-size-fits-all protocol. Clinical judgment and observation lead to the development of exercise programs that induce a mechanical signal at the cellular level. Patient response will determine how much is too much and how little is too little. Clinical research demonstrated, however, that eccentric exercise programs can be quite effective.
Conclusion:
Our traditional views of therapeutic exercise and the treatment of Achilles Tendinopathy must be reconsidered. Exercise is a modality of repair and well as a means of restoring function. Exercise that does not exacerbate pain and other symptoms of inflammation may lead to more rapid tissue repair which can lead to earlier recovery. The deleterious effects of rest and immobilization on tissue health must be balanced against benefits of pain relief and comfort. However, when these guidelines are observed, loading through exercise likely provides the stimulus for repair and recovery in the most efficient manner possible. Tissue loading facilitates repair much better than ice and other bioelectrical modalities.
References
Introduction and Anatomical Overview:
Muscle is made up of two types of fibers, intrafusal and extrafusal. Extrafusal fibers are the contractile fibers and intermixed within the extrafusal fibers are intrafusal fibers. Housed within intrafusal fibers is a specific type of mechanoreceptor. Mechanoreceptors, in general, are interspersed through the entire body – hair, skin, ligaments – and are responsible for sensing tissue pressure and distortion and give our body a sense of proprioception by detecting position of our muscles, bones, and joint. There are many types of mechanoreceptors, but one specifically – the muscle spindle – lives within the intrafusal muscle fibers. The muscle spindle transmits sensory data regarding changes in muscle length, and therefore movement, to the central nervous system (CNS) via the primary afferent (sensory) neurons. The intrafusal fibers receive neural stimulation from gamma efferent (motor) neurons. Think of the gamma motor neuron as a type of sensitivity adjuster. The efferent input adjusts the length of the spindle so that it remains at an optimal length to detect changes within the muscle.
What is Gamma Gain:
Oftentimes, there may be hyperactivity of the gamma motor neurons. This hyperactivity causes continual tightening of the intrafusal fibers, known as gamma gain. Gamma gain leads to hypertonicity in the muscle , causing adaptive shortening of surrounding fascial tissues. These taut bands of fascial tissues lead to hypersensitive trigger points associated with myofascial pain syndrome (MFPS).
The question of what causes gamma gain is unclear. However, acute injury will result in muscular spasm and guarding. Also, pain receptors (nociceptors) increase gamma motor response. Chronic pain, such as that of MFPS is also a result of gamma gain. The aforementioned hyperactivity of the gamma motor neuron, hypersensitivity to stretch and subsequent adaptive tissue shortening becomes hypersensitive to stretch. Stretch of fascial tissue is painful and this results in an increase in gamma motor activity; a vicious cycle of gamma motor hyperactivity, hypersensitivity, hypertonicity, adaptive shortening, and pain. The cycle builds from mild, localized discomfort and will progress to a pain pattern that includes moderate to severe pain with pain referral.
For effective treatment of this persistent pain pattern, therapy must focus on breaking this cycle. Breaking this cycle by blocking gamma gain is the focus of two manual therapy techniques: myofascial release and strain–counterstrain. The positioning for these techniques decrease gamma motor activity and interrupts the cycle.
Myofascial Release:
Many modalities can be used to treat physically active individuals, and all treatment plans for myofascial pain should include active therapeutic exercise. None of these interventions, however, directly address the problem of fascial restrictions and gamma gain.
Myofascial release techniques, more specifically indirect myofascial release techniques, place muscle and fascia in positions that remove stress from the tissues. The application of light, sustained pressure up to the fascial resistance barrier allows the tissue to relax. The shortened position decreases noxious stimulus from the tissue, which in turn diminishes activity in gamma motor nerves. Direct techniques attempt to stretch bound fascia, by applying load through a restrictive barrier. This will decrease the afferent input from the tissue. Both types of techniques can be used to treat myofascial pain pattern, however, the primary focus of the indirect technique is to address gamma gain, by decreasing efferent stimulus.
Strain–Counterstrain:
Strain–counterstrain, originated by Dr. Lawrence Jones, is another type of manual therapy technique that places emphasis on gamma gain. Strain–counterstrain relieves pain and dysfunction by altering neural activity. Strain–counterstrain is a technique in which a body segment is passively moved into a position of least discomfort. Like indirect myofascial release, moving to a position of comfort decreases noxious stimulus from the tissue and diminishes activity of gamma motor nerves, which are responsible for the dysfunction.
Like myofascial release, strain-counterstrain has both direct and indirect techniques. Direct techniques involve applying force against a restrictive barrier to improve motion, whereas indirect techniques involve moving the body away from a motion-restricting barrier to a position of comfort and relaxation. Hold the passive position for a period of 90-120 sec, then slowly move back to a resting, neutral position. Placing a body segment in a position of comfort reduces gamma motor activity which in turn halts the cycle of hypersensitivity, hypertonicity, and adaptive shortening.
Conclusion:
If you have a client complaining of persistent pain patterns similar to myofascial pain syndrome it may be a result of gamma gain. Using manual therapy techniques such as indirect myofascial release and indirect strain-counterstrain may pay big dividends at relieving pain and improving function. Applying these manual therapy techniques in combination with other modalities and therapeutic exercise can have a positive impact on patient outcomes.
A portion of the content contained in this post was adapted from Denegar et, al., Therapeutic Modalities for Musculoskeletal Injuries, 3rd Edition. Human Kinetics
 It’s a shame that a multibillion dollar industry is fueled by misleading people. The business of supplementation is championed by big businesses who utilize fear-mongering tactics to influence the public. These companies disseminate biased data and purport ridiculous claims. ‘We are a nation of rising chronic disease, take this multivitamin.’ ‘We are a nation of malnourished kids, take this multivitamin.’ ‘Autism linked to vitamin deficiency, take this multivitamin.’ ‘Agriculture has ruined our soil; it is depleted of nutrients, take this multivitamin.’ It is an infestation of pseudoscience propaganda that gets delivered daily to our email inbox and shared via social media.
It’s a shame that a multibillion dollar industry is fueled by misleading people. The business of supplementation is championed by big businesses who utilize fear-mongering tactics to influence the public. These companies disseminate biased data and purport ridiculous claims. ‘We are a nation of rising chronic disease, take this multivitamin.’ ‘We are a nation of malnourished kids, take this multivitamin.’ ‘Autism linked to vitamin deficiency, take this multivitamin.’ ‘Agriculture has ruined our soil; it is depleted of nutrients, take this multivitamin.’ It is an infestation of pseudoscience propaganda that gets delivered daily to our email inbox and shared via social media.
Last night, I was in my normal geek mode and came across a news story on my Flipboard feed; Are multivitamins a waste of money? I was glad to see an article disputing the inaccurate claims made by the industry. The article quotes an editorial published in this week’s Annals of Internal Medicine to support the claim that using supplements and multivitamins to prevent chronic conditions is a waste of money.
Hallelujah!
***
Those who follow my blog, know that I strongly believe the body is an amazing system. If that system is treated properly, it can – in most instances – heal organically. You may have read my blog on the overuse of ice and why ice and NSAIDs are not the answer; these posts talk about organic healing of the neuromusculoskeletal system absent of modalities and medicine. I feel the same about nutrition and supplementation.
Last October, I wrote a post titled “Eat This! Don’t take that!”. Our body has always been able to do its job, yet every day nearly three-quarters of the population take a supplement. Multivitamins, fish oil, antioxidants, vitamin D, Vitamin E, B-complex vitamins, conjugated linoleic acid, chromium, pyruvate, CoQ10, etc., Why do we suddenly feel it is necessary to incorporate supplements into our diets?
In most cases a well-balanced diet can provide every nutrient we need  to combat disease. Have you ever watched the TEDx talk “Minding Your Mitochondria” by Dr. Terry Wahls? If not I highly recommend you do (video below). In short, Dr. Wahls is a physician who underwent chemotherapy to treat multiple sclerosis and eventually became relegated to a tilt-recline wheelchair because of weakness. Dr. Wahls made a dramatic transformation, using diet alone. A hearty, vegetable-rich diet reversed her MS. Within a year, she walked without a cane and even completed an 18-hour bicycle ride. Take the time and watch the amazing video.
to combat disease. Have you ever watched the TEDx talk “Minding Your Mitochondria” by Dr. Terry Wahls? If not I highly recommend you do (video below). In short, Dr. Wahls is a physician who underwent chemotherapy to treat multiple sclerosis and eventually became relegated to a tilt-recline wheelchair because of weakness. Dr. Wahls made a dramatic transformation, using diet alone. A hearty, vegetable-rich diet reversed her MS. Within a year, she walked without a cane and even completed an 18-hour bicycle ride. Take the time and watch the amazing video.
***
Back to the editorial piece in the Annals of Internal Medicine. Dr. Edgar Miller, professor of medicine and epidemiology at Johns Hopkins University School of Medicine and co-author of the editorial said, The [vitamin and supplement] industry is based on anecdote, people saying ‘I take this, and it makes me feel better’.
The article goes on to state when you put it to the test, there’s no evidence of benefit in the long-term. It can’t prevent mortality, stroke or heart attack. The editorial was based on three studies, which were also published in this week’s Annals of Internal Medicine.
The first study was a meta-analysis of 27 studies that covered more than 450,000 participants and found that multivitamins had no beneficial effect on preventing cardiovascular disease or cancer. The second study looked at 1,700 patients who previously had heart attacks. They were assigned to take three multivitamins or placebos twice a day for five years. This study was inconclusive. The final study followed nearly 6,000 men older than 65, who took either a multivitamin or a placebo for 12 years. The men were administered cognitive functioning tests, and test results found no differences between the two groups.
All that said most Americans are undernourished. I am the prime example: college football Saturday with wings and beer, the ultimate loaded nacho plate on UFC Fight Night and NFL Sunday Ticket with pepperoni pizza, Pepsi, and popcorn. While I know this is wrong, I also know that an artificial, unregulated multivitamin supplement is not the answer. I might be deficient in a few nutrients, but not completely deficient in all. Maybe my vitamin D intake is only 50% of what it should be, but why should I take a multivitamin that provide me an additional 200%? Wouldn’t I only need an additional 50%? There are toxicity effects to excessive vitamin/mineral intake. I can cause more harm than good by following this concept. If I am that concerned about my health, I need to be a responsible, skip the supplements, and start eating a salad.
 In 2010, I left clinical rehabilitation and performance training. While I love my current job, I do miss the clinical aspect, which is why I seize opportunities to take on random clients with complex issues. I’ve never written about my clients, but this case is so common, yet complex, that I thought my readers might be challenged with similar clients/athletes, or might be experiencing similar issues themselves. Here is a runner’s story that went from marathon training, to painful walking and an inability to run. Her experiences with continued failed treatment and the road we have taken to get her back to training and setting personal records.
In 2010, I left clinical rehabilitation and performance training. While I love my current job, I do miss the clinical aspect, which is why I seize opportunities to take on random clients with complex issues. I’ve never written about my clients, but this case is so common, yet complex, that I thought my readers might be challenged with similar clients/athletes, or might be experiencing similar issues themselves. Here is a runner’s story that went from marathon training, to painful walking and an inability to run. Her experiences with continued failed treatment and the road we have taken to get her back to training and setting personal records.
Her Story
“I was an athlete my whole life, but started distance running in January 2010 to train for my first half marathon. I ran without pain for a year and a half until September 2012 while I was training for my second full marathon. My pain began with a dull knee pain.
I first sought help from the walk in sports medicine clinic. The athletic trainer told me to stretch my hamstrings and gave me a few exercises to strengthen my hips, but told me I could continue running as long as it wasn’t too painful. I followed his advice, but the pain kept getting worse. Subsequently, I made an appointment with an Orthopedist.
The orthopedist diagnosed me with hamstring tendonitis and said I could continue running as long as the pain wasn’t too bad, but that I should work to correct running form. I was referred to another clinical athletic trainer who treated me with muscle stim and recognized weakness in my hips and hamstrings. He suggested that I focus intensely on stretching my hamstrings and that I change my running form from a heel to forefoot strike, to reduce the load on my hamstrings. Following this advice did not help and eventually pain developed in the neck and mid-back.
I just kept getting new pain – neck, mid-back, lower back, hips, and hamstrings. The only thing that felt ok was walking—but eventually the sharp pain in my hips even limited my ability to walk. At this point I grew concerned and made an appointment with my primary care physician in March, who did some lab work but didn’t find anything. That physician referred me to a physical therapist, but he didn’t feel comfortable prescribing much of anything, since both back flexion and extension were causing me pain. Eventually the postural training failed as well.
After 6 months of pain and 3 months of, on again / off again training, I became miserable and desperate. I stopped all training in early to mid-March.”
My Assessment
She outlined a history, as summarized above, however, something very unique to her was she was diagnosed with a hormonal imbalance, which as you will read, comes in to play later. I performed a physical examination and found special tests for soft and bony tissue to be unremarkable. Thus, far she had non-specific multi-segmental pain. Her pain patterns and complaints were so indistinct that I even evaluated for potential malingering using Gordon Waddell’s (1980) non-organic pain patterns. This too was negative.
I did a full body movement assessment to evaluate for potential arthokinematic and neuromuscular dysfunction. If dysfunction were present specific compensatory patterns would emerge. This assessment was positive for a large number of breakdowns in the kinetic chain. Through the entire evaluation I identified the following arthrokinematic and neuromuscular dysfunctions.
|
Arthrokinematic |
Neuromuscular |
||
|
Hypomobility |
Hypermobility |
Hypotonicity |
Hypertonicity |
|
Ankle dorsflexion |
Forefoot pronantion |
Medial calf (gastrocnemius, post/ant. Tibialis) |
Lateral calf and peroneals |
|
Knee extension |
SI joint / Pelvis (anterior innominate rotation + pelvic upslip) |
Medial hamstrings |
Biceps femoris |
|
Hip extension |
scapulothoracic |
Adductor magnus |
Adductor group (not magnus) |
|
Thoracic Spine |
Lumbar spine |
Gluteal group |
Hip flexors |
|
Glenohumeral |
Cervical spine |
Transverse abdominus |
Rectus abdominus |
|
1st Rib |
Right external oblique and left internal oblique |
Quadratus Lumborum |
|
|
Rhomboid/middle/lower trapezius |
Pec major and pec minor |
||
|
Deep cervical flexors |
Levator scapula and upper trapezius |
||
|
Scalenes / sternocleidomastoid |
|||
Overall, she had signs and symptoms of many injuries; from facet arthropathy to PFPS to cervical dystonia, but rather than treat the injury, I only cared about the dysfunction and treated as such.
Phase I – Correct Dysfunction (6 weeks)
We worked 3-5 days per week correcting imbalances. I addressed the above mentioned neuromuscular hypertonicity using, muscle energy, active release technique, positional release technique, and myofascial release. I coupled the neuromuscular work by applying joint mobilizations or Mulligan’s mobilizations to hypomobile joints. Together this treatment would increase dynamic range of motion.
using, muscle energy, active release technique, positional release technique, and myofascial release. I coupled the neuromuscular work by applying joint mobilizations or Mulligan’s mobilizations to hypomobile joints. Together this treatment would increase dynamic range of motion.
When decreasing neural impulse to hypertonic muscles it is prudent to increase neural drive to the hypotonic muscles. This was done with focused isolated strengthening of weak muscles and positional isometrics. I also added light multi-segmented strengthening to facilitate neuromuscular control through dynamic and multi-planar movement.
As you can see this is a lot of work and obviously we could not do all of this every single day. We targeted the biggest issues and switched it up from day to day. Each session would last 45-60 minutes. We remained in this phase for approximately 6 weeks. By the end of this phase I no longer had to perform manual therapy.
Phase II – Continue corrective, increase strength, re-introduce running
Once we had corrected the imbalance, the goal is to increase neuromuscular demand while ensuring proper mechanics during movement was maintained. A simple periodization program alternating between corrective exercise and strengthening was applied. For example, the corrective day might include single leg bridge, clams, and ball Y’s and T’s. The strengthening day, might include, single leg squats, RDLs and seated rows.
Because we had corrected muscle imbalance we could now reintroduce running. The goal for running was threefold: 1- reestablish cardiorespiratory endurance. 2- Ensure the corrective exercise done in phase 1 was good enough to maintain proper mechanics while running and 3- to see if she can perform pain free running. We began with slow, steady state cardio programming. All training runs were preceded by 15-20 minutes of corrective exercise.
At first it was no more than 1 or 2 miles per week. We ramped this up pretty quickly as tolerated. By the end of another 4-6 weeks (early/mid-August) we would get to 3 mile runs and up to 6-7 miles per week. She did not run faster than a 9:30 pace. There would be occasional set-backs lasting 24-72 hours and discovered that she may need longer recovery periods.
This is where her physician-diagnosed hormonal imbalance came in to play. The pituitary gland, specifically the anterior lob, is responsible for secretion of somatotrophins or more commonly known as human growth hormone. With suppressed hormonal secretion her body is subject to slight delays in tissue regeneration. Subsequently, we have a cascade effect of tissue breakdown that is unable to regenerate as fast as normal, which can lead to injury. To combat this, we had to allot for more recovery time between training days.
Phase III – Continue corrective, continue strength, and introduce power and speed
 By now, she had regained enough motor control and demonstrated neuromuscular command that we can begin incorporating higher intensity work like power, speed, agility, and quickness (SAQ) training. We did not forget what we had done in phase I and Phase II and would continue performing these exercises 1-2 days per week. The primary objective when performing power, speed, quickness, and strengthening was to ensure she did not demonstrate poor movement patterns. If she did, the exercise was too intense and needed regression. The secondary objective was performance enhancement.
By now, she had regained enough motor control and demonstrated neuromuscular command that we can begin incorporating higher intensity work like power, speed, agility, and quickness (SAQ) training. We did not forget what we had done in phase I and Phase II and would continue performing these exercises 1-2 days per week. The primary objective when performing power, speed, quickness, and strengthening was to ensure she did not demonstrate poor movement patterns. If she did, the exercise was too intense and needed regression. The secondary objective was performance enhancement.
An example of exercises we might perform in this phase are power step-ups, box jumps, split squat jumps, ice skaters, and speed ladder work. The speed and intensity at which we perform these exercises were dependent on her ability to control the movement with proper mechanics and muscle firing patterns. Again we followed an undulating periodization approach, where corrective, strength, speed, and power work was alternated throughout the week.
We also began to increase running intensity and distance. We began with short tempo and interval training runs. The goal was to reduce her pace from 9:30-10 minutes / mile down to 8:15-8:45 minutes/mile. While rest and inactivity does lead to overall deconditioning, it takes longer for the cardiorespiratory system to become deconditioned when compared to the neuromuscular system. Thus, getting her back to an 8:30 mile pace was fairly easy to achieve. As tolerated we introduced longer runs (5-6 miles). At the end of this phase, I felt confident enough to challenge running to a pre-injury pace. This meant running a 5k at sub 24 minutes.
Phase IV – Performance development (our current phase)
This is the final phase. As of mid-October, we have scaled back substantially on corrective exercise (although, we still do it on occasion) and have primarily been focused on performance gains. Daily workouts are now focused on strength, power, and SAQ. No matter what, all training sessions begin and end with foam rolling and stretching (either static, active, or dynamic).
We have slowly increased pace of runs through manipulation on/off times and intensity, and she is now back to pre-injury running pace. In the coming weeks and months we will continue to work toward half- marathon distance and increase speed over the duration of 13.1 miles. We have two ultimate goals that I am optimistic we will achieve: Continue pain free running and set a PR in the Illinois half marathon on April 26, 2014.
A post write-up unsolicited testimonial
I am amazed at the progress we have made over the past 6 months without surgery, drugs, bracing, taping, or even ice. I am a stronger athlete now than I ever was, and hope others who relate to my case can benefit from Josh’s extensive knowledge and dedication to treating his clients.
In July I posted a blog discussing the overuse of cryotherapy. The controversy surrounding the topic made it one of the most popular blogs I’ve written. What is surprising to me is that a controversy exists at all. Why, where, and when did this notion of anti-inflammation start? Ice, compression, elevation and NSAIDs are so commonplace that suggesting otherwise is laughable to most. Enter an Athletic Training Room or Physical Therapy Clinic nearly all clients are receiving some type of anti-inflammatory treatment (ice, compression, massage, NSAIDs, biophysical modalities, etc). I evaluated a client the other day and asked what are you doing currently – “Well, I am taking anti-inflammatories and icing.” Why do you want to get rid of inflammation and swelling? I ask this question for both chronic and acute injury!
The Stigma of Inflammation
Editor in Chief of The Physician and Sports Medicine Journal (Dr. Nick DiNubile) once posed this question: “Seriously, do you honestly believe that your body’s natural inflammatory response is a mistake?” Much like a fever increases body temperature to kill off foreign invaders; inflammation is the first physiological process to the repair and remodeling of tissue. Inflammation, repair, and remodel. You cannot have tissue repair or remodeling without inflammation. In a healthy healing process, a proliferative phase consisting of a mixture of inflammatory cells and fibroblasts naturally follows the inflammatory phase (1).
Researchers headed by Lan Zhou, MD, PhD, at the Cleveland Clinic, found that in response to acute muscle injury, inflammatory cells within the damaged muscle conduct phagocytosis, contribute to accumulation of intramuscular macrophages, and produce a high-level of Insulin-like growth factor 1, (IGF-1) which is required for muscle regeneration (3). IGF-1 is a primary mediator of the effects of growth hormone and a stimulator of cell growth and proliferation, and a potent inhibitor of programmed cell death. Similarly, in 2010, Cottrell and O’Conner stated “overwhelmingly, NSAIDs inhibit or delay fracture healing” (2). And you want to stop this critical process of healing by applying ice, because inflammation is “bad”?
The Anecdotal Rationale for Ice
Somewhere along the line the concept that ice facilitates healing became conventional wisdom. Sorry, that wisdom is wrong. I had someone tell me the other day, “We need to ice, because we need to get the swelling out.” Really? Does ice facilitate movement of fluid out of the injured area? No, it does not. The lymphatic system removes swelling. The Textbook of Medical Physiology says it best:
“The lymphatic system is a ‘scavenger’ system that removes excess fluid, protein molecules, debris, and other matter from the tissue spaces. When fluid enters the terminal lymphatic capillaries, any motion in the tissues that intermittently compresses the lymphatic capillaries propels the lymph forward through the lymphatic system, eventually emptying the lymph back into the circulation.”
Lymphatic drainage is facilitated by contraction of surrounding muscle and changes in compressive forces that push the fluid back to the cardiovascular system. This is why ankle pumps works so well and removing swelling accumulation.
Besides, since when is inflammation a bad thing? Inflammation is a necessary component in the first phase of phase of the healing process. Swelling is controlled by the body’s internal systems to attain homeostasis. If swelling is accumulated it is not because there is excessive swelling, rather it is because lymphatic drainage is slowed. The thought that ice application increases lymphatic flow to remove debris makes no sense. Gary Reinl, author of “Iced! The Illusionary Treatment option gave me a good analogy. Take two tubes of toothpaste, one is under ice for 20 minutes, the other is warmed to 99 degrees. In which tube will the toothpaste flow fastest? It does not take an advanced physics degree to know that answer.
What might surprise you is that ice actually reverses lymphatic drainage and pushes fluid back to interstitial space. A study published in 1986 (yes, 1986, is old, but this is a foundational study) found when ice is applied to a body part for a prolonged period of time; lymphatic vessels begin to dramatically increase permeability. As lymphatic permeability increases fluid will pour from the lymphatics into the injured area, increasing the amount of local swelling (5). Ice can increase swelling and retard debris removal!
Load Facilitates Repair
The acronym RICE is bogus in my opinion. Rest is not the answer. Rest does not stimulate tissue repair. In fact rest causes tissue to waste. The other reason RICE is bogus is obvious, ice. Evidence has shown that tissue loading through exercise or other mechanical means stimulates gene transcription, proteogenesis, and formation of type I collagen fibers (See studies by Karim Khan, Durieux, Mick Joseph, and Craig Denegar). Ice does nothing to facilitate collagen formation.
Our body has all types of cells. When a cell is born it has no clue what type of cell it will eventually become. This infancy cell – for lack of a better term – is called a progenitor cell. Progenitor cells can be changed to a specific cell type. Load in tendon tells our body to turn a progenitor cell in to a tenocyte. Load in bone tells a progenitor cell to become an osteocyte. Ever wonder why myositis ossificans (calcification or bone growth in muscle) develops? The direct, repeated trauma turns progenitor cell currently living within muscle to an osteocyte. Subsequently, we develop bone growth within muscle.
Ice will not influence progenitor cells development. Ice does not regenerate tissue. Ice does not facilitate healing – it inhibits natural healing process from occurring. Ice does not remove swelling; it increases swelling and lymphatic backflow.
Closing thoughts
Bottom line, ice and NSAIDs are over utilized. I am not saying never, but I am saying ice is not a magical cure all that fixes everything and is required for healing. It is not the gold standard that it has come to be. My goal with this blog is to get individuals to stop and think before immediately turning to ice and NSAIDs. Is it really the best option? Is it necessary for this injury at this stage? I understand it is not the only form of treatment clinicians use, but ice certainly is the most heavily used. My goal is to get this trend reversed one clinician and one patient at a time. Have you seen the video discussion between Kelly Starrett, DPT and Gary Reinl? If not I recommend you watch it. It’s fascinating. I am glad to have expert minds like Kelly and Gary in this fight with me.
I ask health care professionals to do one thing, just try it. Pick one client with chronic musculoskeletal pain, skip the ice, skip the NSAIDs and try to use light exercise as a repair stimulus. Then, try skipping the ice on a client with an acute mild injury. The outcomes might surprise you.
Great Thought Provoking Reads
Hart JM, Kuenze CM, Pietrosimone BG, Ingersoll CD. Quadriceps function in anterior cruciate ligament-deficient knees exercising with transcutaneous electrical nerve stimulation and cryotherapy: a randomized controlled study. Clin Rehabil. 2012 Nov;26(11):974-81.
**Update**:
I’ve had an enormous amount of feedback for this post. I greatly appreciate all of it – good and bad. I am adding this note in regards to an overwhelming amount of questions / comments about acute injury and other treatment options.
In regards to acute injury, my response is yes, in many cases I would skip the ice for acute injuries as well!! Why do you feel like we must ice an acute injury but not ice the chronic? What is the benefit to halting the healing process of an acute injury? To prevent hypoxic death or to reduce pain? We’d have hypoxia with or without ice. The body will remove dead cells and replenish with new. I agree, ice has pain modulating effects. But to this I ask, at what cost are we reducing the pain? Is a temporary (30 minutes) pain reduction more important than healing? Theoretically, pain can increase after icing secondary to the back flow of lymphatic drainage that may further increase post-ice swelling.
The second set of comments I receive are regarding topics like heat, other modalities, what would I do in situation x, or ice is not all we do. I understand this, but these are beyond the scope of this blog. If I wrote to each point I’d be authoring a textbook rather than a blog post. Hopefully, I can touch on these topics in later posts.
References
EXSS is Exercising Science Solutions for Public Impact
Hannah Park
Active Living, Active Healthcare
West Boylston, MA | Powerlifting | Strength Training
Incorporating Critical Thinking into Physical Therapy Practice
adventures in bringing the DAT to life... "No man ever steps in the same river twice, for it is not the same river and he is not the same man."-Heraclitus of Ephesus
Daily choices and habits to create wellness, fitness and health.